Vitiligo: the gut microbiota at the heart of skin oxidative stress
The gut microbiota may play an important role in the onset and progression of vitiligo. Hippuric acid, a metabolite produced by the microbiota, may be a key mediator of oxidative stress… and a potential biomarker or even a therapeutic target?
Lay public section
Find here your dedicated section
Sources
This article is based on scientific information

About this article
Vitiligo, an autoimmune skin disease, is characterized by the destruction of melanocytes, leading to depigmented patches. However, cutaneous oxidative stress—a key factor in the progression of the disease—appears to be influenced by the gut microbiota. Here’s a breakdown of a study that examines the mechanisms at work.1
Oxidative stress linked to the gut microbiota
The first step in the researchers’ work involved analyzing lesions in patients and in a mouse model. This revealed, in the depigmented areas, an overexpression of genes associated with oxidative stress and responses to reactive oxygen species (ROS). This confirms that these processes are crucial in the pathogenesis of the disease.
Next step: the researchers discovered that mice with vitiligo exhibit a significant accumulation of ROS in the skin, as well as mitochondrial abnormalities in their melanocytes. Eliminating the gut microbiota with antibiotics reduced the abnormal accumulation of ROS and the mitochondrial abnormalities in the melanocytes, resulting in a significant improvement in depigmentation. Thus, the gut microbiota appears to directly regulate the skin’s oxidative stress status.
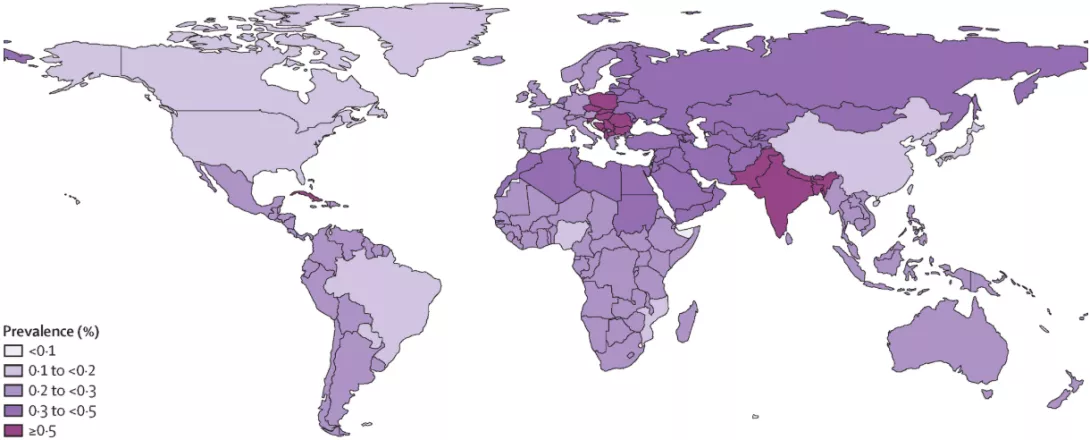
Vitiligo around the world
- The global lifetime prevalence of vitiligo diagnosed by a physician or dermatologist is estimated at 0.36% in the general population, 0.67% in the adult population, and 0.24% in the pediatric population.2
- Among adults, prevalence estimates range from 0.43% in East Asia to 0.98% in Central Europe.2
- Among children, the prevalence of vitiligo ranges from 0.16% in East Asia to 0.35% in South Asia and 0.35% in Central Europe.2
From the gut microbiota to the skin
Subsequent research by scientists shows that the microbiota of mice with vitiligo is imbalanced (increased Clostridiales, decreased Verrucomicrobiae). Transferring this dysbiotic microbiota (through cohabitation of animals or fecal transplantation) exacerbates depigmentation. Conversely, administering probiotics slows the progression of the disease, suggesting a potential therapeutic approach.
But how is the gut microbiota linked to the skin? Metabolomic analysis of fecal, blood, and skin tissues from mice identified a key factor: hippuric acid, a metabolite derived from the microbiota, accumulates excessively in the feces, serum, and skin of mice with vitiligo. Injections of hippuric acid are sufficient to reproduce the accumulation of ROS and exacerbate depigmentation in mice. And in humans? Serum levels of hippuric acid are found to be higher in patients with vitiligo.
A mechanistic hypothesis
This leads to the following hypothesis: in mice with vitiligo, the intestinal mucosal barrier is weakened (due to a reduction in goblet cells responsible for mucus production and a decrease in mucosal thickness), which increases intestinal permeability. This increased permeability would facilitate the passage of hippuric acid into the bloodstream and then to the skin. Hippuric acid would induce oxidative stress by directly binding to two proteins (NOS2 and MAPK14); this direct molecular interaction would then promote the production of ROS in skin tissues.
Thus, intestinal dysbiosis would orchestrate cutaneous oxidative stress in vitiligo via hippuric acid. These results also suggest that probiotics may play a role in slowing the progression of the disease.