Symptom-specific gut microbial and metabolic profiles in ADHD reveal SCFA deficiency as a key pathogenic mechanism
By Prof. Emmanuel Mas
Gastroenterology and Nutrition Department,
Children’s Hospital, Toulouse, France
Comments on the original article by Wang et al. (Gut Microbes 2025) 1
Lay public section
Find here your dedicated section
Sources
This article is based on scientific information
Sections

About this article
Previous evidence links gut microbiota to attention-deficit/ hyperactivity disorder (ADHD) through the gut-brain axis. However, the specific microbiota contributing to symptoms remain unclear. To characterise the gut microbial profile linked to different symptoms and explore the mediation mechanism between microbiota alterations and the main ADHD symptoms, the authors of the article conducted shotgun metagenomic sequencing and faecal metabolomics analysis on 94 ADHD patients and 94 age- and gender-matched controls. They analysed the microbial characteristics of three subgroups presenting with different main
symptoms of ADHD. Faecal microbiota transplantation in mice validated the hypothesis that gut microbial composition affects ADHD symptoms through metabolic alterations. This study provided further insight into the mechanisms underlying metabolic disturbances in ADHD and shed light on the role of gut microbiota in these processes.
What do we already know about this subject?
Attention deficit hyperactivity disorder (ADHD) is common in paediatrics, with a 3-5% prevalence. Various environmental factors play a role in the development of ADHD, including perinatal, social-emotional and nutritional factors. These risk factors also influence the gut microbiota (GM). Early alterations can disrupt neurological development. These effects could be mediated by the microbiota-gut-brain axis through three pathways (immune, neuronal and endocrine/systemic).
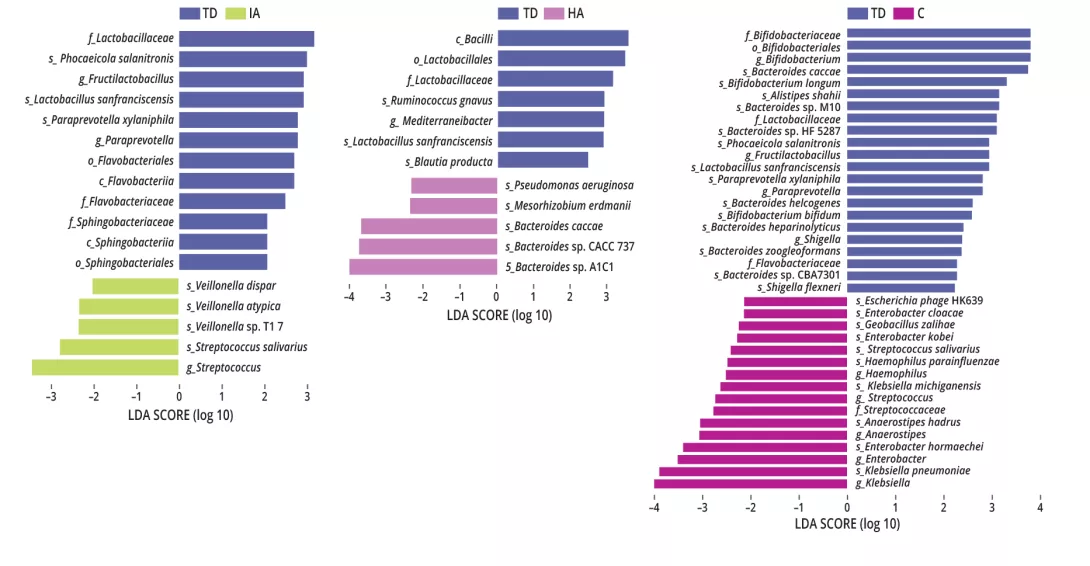
Figure 1 - Specific differences in bacterial taxa between each of the ADHD groups.
What are the main insights from this study?
One hundred and eighty-eight (188) children were included in a single-centre Chinese study, including 94 children with ADHD who were divided into three subgroups, 56 with predominant inattention symptoms (group IA), 9 with predominant hyperactivity-impulsivity symptoms (group HA) and 29 with combined symptoms (group C), and 94 controls (group TD).
The GM analysis found no difference between these three groups in terms of bacterial richness and diversity, the relative abundance of the 10 main genera and the Firmicutes/Bacteroidetes ratio. However, specific taxa were associated with ADHD subtypes (figure 1).
The GM analysis found no difference between these three groups in terms of bacterial richness and diversity, the relative abundance of the 10 main genera and the Firmicutes/Bacteroidetes ratio. However, specific taxa were associated with ADHD subtypes (figure 1).
The family Lactobacillaceae and species Lactobacillus sanfranciscencis were enriched in the TD group. The TD group had more Bifidobacteriales than group C. In groups IA and C (inattention symptoms), the genus Streptococcus and species Streptococcus salivarius were identified as harmful bacteria, while family Flavobacteriaceae, genus Paraprevotella, genus Fructilactobacillus, species Paraprevotella xylaniphila, and species Phocaeicola salanitronis were beneficial. In groups HA and C (hyperactivity-impulsivity symptoms), the family Lactobacillaceae and species Lactobacillus sanfranciscencis were beneficial (figure 1).
The metabolomic profiles of ADHD children revealed disturbances in fatty-acid synthesis, with a significant reduction in the synthesis of unsaturated fatty acids and linoleic acid, as well as amino-acid metabolism (figure 2). The various symptoms, inattention, hyperactivity and impulsivity, were negatively correlated with different metabolites, imidazoleacetic acid and inattention (p<0.001). Thus, Lactobacillus
sanfranciscencis had a direct effect and an effect mediated by imidazoleacetic acid on inattention.
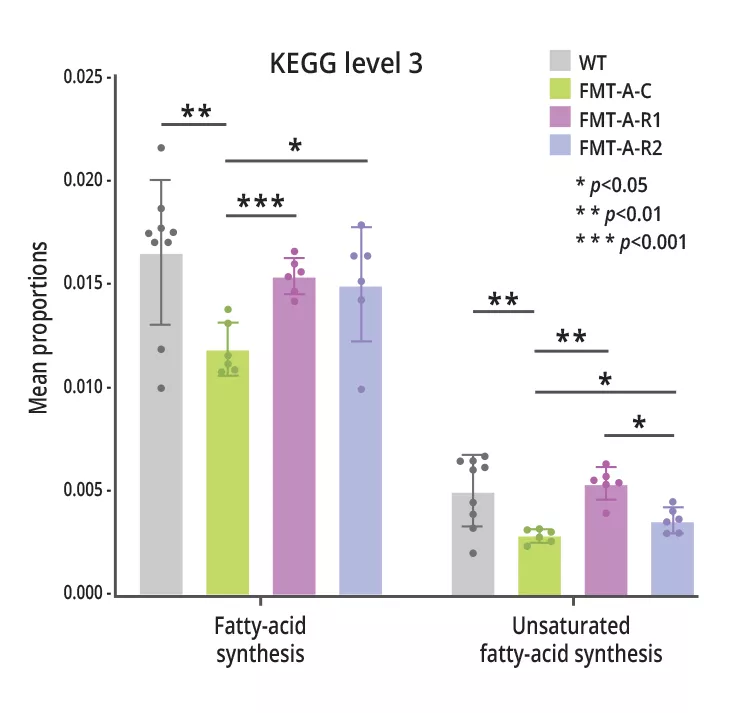
An experiment with three cycles of faecal microbiota transfer (FMT) from children with ADHD and a low abundance of beneficial Lactobacillus sanfranciscencis bacteria (FMT-A group) and controls (FMT-H group) was conducted in four-week-old male C57BL/6J mice. The mice then received either Lactobacillus sanfranciscencis (1 x108 organisms/mouse/day, group FMT-A-R1), or 150 mmol/L sodium acetate (group FMT-A-R2) or PBS for the controls (group FMT-A-C). Hyperactivity symptoms improved significantly in the FMT-A-R1 group but not in the FMT-A-R2 group, while inattention symptoms improved in both groups. Finally, fatty-acid and unsaturated
fatty-acid synthesis was improved in the FMT-A-R1 and FMT-A-R2 groups versus FMT-A-C (figure 3).
Figure 2 - Alteration of the different metabolic pathways, size of the circles corresponding to the number of genes involved.
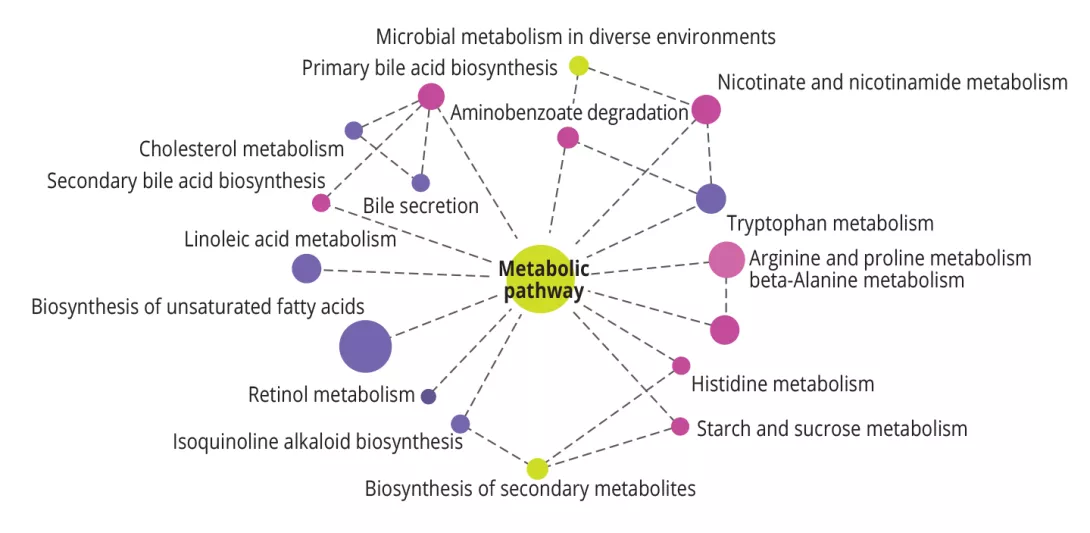
Figure 3 - Faecal transplantation with stools from ADHD children reduces fatty-acid synthesis, which is corrected by treatment with Lactobacillus sanfranciscencis or sodium acetate.
What are the consequences in practice?
This study showed that GM alterations in ADHD children were symptom-dependent. The sub-group analysis showed that family Lactobacillaceae and species Lactobacillus sanfranciscencis were enriched in the TD group. In addition, after faecal transplantation with ADHD stools, treatment with Lactobacillus sanfranciscencis improved symptoms.
Fatty-acid and unsaturated fatty-acid synthesis was reduced in ADHD children. Similarly, after faecal transplantation with ADHD stools, treatment with short-chain fatty acids (imidazoleacetic acid) led to an improvement in symptoms.
- Gut microbiota alterations are specifically associated with the different symptoms of ADHD children. This effect is mediated by disturbances in fatty-acid metabolism
CONCLUSION
The findings of this study add to our understanding of the role the gut microbiota plays in children with ADHD, with metabolic
alterations involved in the disturbance of the microbiota-gutbrain axis in this context.

